As the year comes to an end, I usually look back on what has happened and forward to the coming year.
Over all 2012 was a good year. I started a book on CRPS/RSD which I hope will be published this coming spring. Fellow RSDers and I have started a non profit to help those unable to get treatment financial help. Here is the link:
www.crpspartnersinpain.com
Personally, I learned that I will be a first time grandmother in March 2013.
I have met wonderful people who have responded to this blog or to the Facebook groups where I am an admin.
Ketamine Klub For CRPS/RSD Patients
Ketamine Klub 2 For CRPS/RSD Patients monitored by Dr. Pradeep Chopra
Caregivers of CRPS/RSD Patients
Teen To Thirty: CRPS/RSD Support
We are raising awareness and informing the public about CRPS treatments, feeling and caring for someone with CRPS.
2013 is right around the corner. Through the above organizations, my book and non profit I hope to positively influence those who have CRPS, those who know nothing about CRPS as well as educations physicians of caring for the CRPS patient.
Merry Christmas and a Happy Healthy 2013!!
These are my experiences with RSD, it's symptoms, treatments and how it affects our lives.
Sunday, December 16, 2012
Wednesday, November 14, 2012
CRPS Awareness Month
Wow! It is hard to believe that November is half over. November is CRPS Awareness month. I am currently in the hospital for migraine treatment. Every nurse and doctor who enters my room gets my CRPS Speach.
The book that I have been writing has taken me away from my blog. It should be published in early 2013. I am also working on starting a non profit to help those whose insurance doesn't cover their treatments. I talk to people every day who aren't getting treatment for a variety of financial reasons.
Please help me to spread CRPS Awareness this month.
The book that I have been writing has taken me away from my blog. It should be published in early 2013. I am also working on starting a non profit to help those whose insurance doesn't cover their treatments. I talk to people every day who aren't getting treatment for a variety of financial reasons.
Please help me to spread CRPS Awareness this month.
Thursday, September 6, 2012
Involved in a legal issue regarding RSD?
If you are involved in litigation surrounding your RSD, you might want to look into having a life care planner who specializes in RSD to assist you in your fight. There is an excellent article about it at RSDSA.org. ( http://rsds.org/4/resources/Life_Care_Plans.html)
It is an important part of your case to show what treatments you are likely to need while living with RSD. Check it out.
It is an important part of your case to show what treatments you are likely to need while living with RSD. Check it out.
Follow up on Carpal Tunnel Surgery
I haven't been blogging because my RSD spread into my hand after the carpal tunnel surgery. I knew going into this surgery that there was a 50% chance of spread but my doctor thought that by getting Ketamine during the surgery and immediately after that this would prevent spread. Well it did not.
I was started on LDN (Low Dose Naltrexone - www.ldn.org) and got another round of Ketamine. Two and a half months after the surgery, my hand is improving. A great weight has been lifted for me. I depend on my upper body to compensate for lower extremity RSD. Not being to use my dominant hand was an experience that I never want to repeat.
I was started on LDN (Low Dose Naltrexone - www.ldn.org) and got another round of Ketamine. Two and a half months after the surgery, my hand is improving. A great weight has been lifted for me. I depend on my upper body to compensate for lower extremity RSD. Not being to use my dominant hand was an experience that I never want to repeat.
Tuesday, August 7, 2012
Carpal Tunnel Syndrome Surgery
It has been a while since I have posted. My worst nightmare came true following the carpal tunnel release
Friday, July 6, 2012
The Carpal Tunnel Release Surgery and RSD
High Dose Ketamine and CRPS/RSD Spread
Wednesday June 20th, I finally had my carpal tunnel release surgery with the wonderful Dr. Brian Leung. I had it arranged that I would get 100 mg of Ketamine during the surgery and would then drive down to Miami for high dose Ketamine with Dr Denmis Patin the following week.
The risk of spread of the RSD from carpal tunnel release surgery is 50%. My dilemma was that I was losing function of my right hand due to the carpal tunnel syndrome. I was having difficulties doing my activities of daily living. So if I didn’t do the surgery, I could totally lose function of my dominant hand. If I had the surgery and the RSD spread to my hand, I would not only lose function but have pain as well. After talking to my RSD neurologist, we decided that the risk would be greatly reduced if I had Ketamine during and after the surgery. Of course he could not make a promise that I still wouldn’t have RSD spread; there are no promises when it comes to this disease. I weighted the risks and benefits and decided to have the surgery.
I had arrangements made for a friend to drive me to and from the surgery and another friend to accompany me to Miami for the Ketamine as it is required that someone spend the night with you after the infusion. Two weeks prior to the surgery, the friend who was going to go to Miami with me had a person issue come up and all of a sudden, I had no one to spend the night with me. Fortunately I was able to get another friend to stay with me. She lives in Miami so I would make the drive to and from Orlando on my own.
The surgery went well. I was in a bit more pain than I expected, but nothing that I could’t handle. It did cause a flare in my RSD however. I expected that. I had hoped that by getting the Ketamine during the surgery that I wouldn’t flare, but for me 100 mg isn’t enough to prevent me from flaring.
Sunday, I headed down to Miami driving through tropical storm Debby. That was a harrowing drive. I was never more relieved than when I pulled up in front of the Spring Hills Suites!!
Monday through Wednesday, I got 200 mg per hour of Ketamine along with IV Versed and IV Ativan. The resident was wonderful as is the nursing staff at Sylvester Cancer Center’s Surgical Center. I can not say enough about the staff there!! The resident made sure that I was asleep the entire time so that I would not have any negative side effects from the Ketamine.
When I got home, I still had a suture in my wrist and was still having some burning pain. I rubbed my Ketamine cream into my hand four times a day. Within 48 hours, the burning was gone and although I was still having surgical pain it was soothed by NSAIDs.
Tuesday July 3rd, I saw the surgeon and the suture was removed. I had my first OT session. I realized during the OT session how far I have to go to get full range of motion back. During this week doing the home exercises, I have already seen improvement.
Thanks to a great surgeon, high dose Ketamine and now OT, I feel confident that I made the right decision to have the carpal tunnel release surgery with the high dose Ketamine.
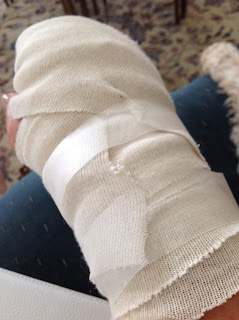
Immediately after surgery this is what my hand looked like
This is my hand July 6, 2012 sixteen days after surgery and a week after high dose Ketamine.
Immediately after surgery this is what my hand looked like
This is my hand July 6, 2012 sixteen days after surgery and a week after high dose Ketamine.
Wednesday, May 23, 2012
I'm normal, not a celebrety or a monster!
I'm in Miami helping someone with RSD get her Ketamine, just as she helped me in March. There are some members on an online group that I belong to staying here as well. Some were anxiou to meet me, which was flattering. One young member treated me like a celebrety. Then there are others, who think that I'm an egomaniac when I share the history of Ketamine in Philadelphia (and possibly the US) of which I happen to be a part of. As a nurse, we are trained to teach people about their treatments including the history, of which I just happened to live.
I'm just a normal person like the other members with RSD. I have good days and bad ones. Stress aggravates my condition just like everyone else. I'm a normal person trying to use my nursing education to educate and help others. It DOES make me feel useful for the first time since I had to stop working five and a half years into RSD. If that is wrong, then I'm sorry!
I miss my little group and desperately want to return but without being added to this group and that group without my permission. I don't know if that is possible. Should I start my own secret group with people that I know and trust? But then I'm not reaching the newly diagnosed or the people who need help. Do I branch out and not just do Ketamine? The admins of the K Klub have that under control. So many decisions, but for now, I'm off to Seattle Sunday to get onto the Disney Wonder on Monday headed to Alska to celebrate my 55th birthday.
I return to the Internet June 6th, not as a celebrety or a monster but as a normal person with RSD, who is a nurse, a wife or 34 years, a mom of 31 years and someone who some times cares too much.
(((hugs)))
Saturday, May 19, 2012
Wednesday, May 16, 2012
I Thought I'd Heard It All!
I've had doctors tell me that RSD can't spread, that it is "all in your head", and many other falsehoods but last week I heard something that blew me away. It was so off the wall that I just had to chuckle.
My migraine neurologist wanted me to go to a DO for a Osteopathic Manipulation Treatment. His office made an appointment with a doctor who he recommended. This neurologist is the head of the FL DO association so one would think that he has a good knowledge base but he is one of those neurologists who says that RSD can't spread so I should have known that the DO diagnostician that he sent me to might not know much about RSD either.
When I arrived, they asked for my history. When I went in to see the doctor, she began the manipulation. As she was manipulating my head, she was telling me how she took her son to see a doctor in Chicago who was doing this new injection treatment for neuro-inflammation. She wanted to be sure that I knew that RSD fell into the category of neuro-inflammation. I reminded her that I was a nurse and that I had had RSD for 16 years. She went on to tell me about how this treatment involves the injection of D5W (5% Dextrose in water) into the inflamed nerves. Because of the allodynia on the top of my foot, she wanted to inject the scars from my surgery to fuse my right foot with the D5W (sugar water) to "cure" my RSD. It took every ounce of restraint for me not to laugh out loud right there.
At the end of the treatment, she wrote down the web site of this doctor so that I could check it out. I thanked her and quickly exited. When I went to check out, they wanted me to make an appointment for Monday (this was Friday). I told the receptionist "I don't think that I will be coming back, thank you" and ran out of the door.
I can not see how any physician can believe that 5% sugar water can reverse nerve damage when it is injected into a 15 year old surgical scar. It has to be the wildest "cure" that I have heard for this poorly understood disease. I wonder how many people who are desperate for anything that might help them would pay good money for something like this? She told me that there is no procedure code for this injection. Gee, I can't imagine why! So, she was trying to figure out what to charge for it. You couldn't pay me to let her stick a needle into my RSD foot.
My migraine neurologist wanted me to go to a DO for a Osteopathic Manipulation Treatment. His office made an appointment with a doctor who he recommended. This neurologist is the head of the FL DO association so one would think that he has a good knowledge base but he is one of those neurologists who says that RSD can't spread so I should have known that the DO diagnostician that he sent me to might not know much about RSD either.
When I arrived, they asked for my history. When I went in to see the doctor, she began the manipulation. As she was manipulating my head, she was telling me how she took her son to see a doctor in Chicago who was doing this new injection treatment for neuro-inflammation. She wanted to be sure that I knew that RSD fell into the category of neuro-inflammation. I reminded her that I was a nurse and that I had had RSD for 16 years. She went on to tell me about how this treatment involves the injection of D5W (5% Dextrose in water) into the inflamed nerves. Because of the allodynia on the top of my foot, she wanted to inject the scars from my surgery to fuse my right foot with the D5W (sugar water) to "cure" my RSD. It took every ounce of restraint for me not to laugh out loud right there.
At the end of the treatment, she wrote down the web site of this doctor so that I could check it out. I thanked her and quickly exited. When I went to check out, they wanted me to make an appointment for Monday (this was Friday). I told the receptionist "I don't think that I will be coming back, thank you" and ran out of the door.
I can not see how any physician can believe that 5% sugar water can reverse nerve damage when it is injected into a 15 year old surgical scar. It has to be the wildest "cure" that I have heard for this poorly understood disease. I wonder how many people who are desperate for anything that might help them would pay good money for something like this? She told me that there is no procedure code for this injection. Gee, I can't imagine why! So, she was trying to figure out what to charge for it. You couldn't pay me to let her stick a needle into my RSD foot.
Tuesday, April 3, 2012
Ketamine With A New Doctor
My Ketamine care has been under the guidance of Dr S in Philadelphia since October 2011. He sent me to Germany on October 2011 for my coma treatment and orchestrated the outpatient infusions at Cooper Medical Center beginning in February 2002. He has now turned over my Ketamine care to a doctor in Miami FL. The reason for this is two fold; Dr S is now in his 70's and his patient load is getting so large that he is trying to find local doctors for his out of town patients to manage their Ketamine care.
A week before I was scheduled to drive down to Miami with a nurse who I met through this blog (Christina) who also lives in the Orlando area, I had a really bad fall. I was taking my dog Nemo across the street to the grassy area of our cul de sac to do her business when my foot just gave out. My foot has a history of doing this. Because of my carpal tunnel syndrome, I can't use a cane or a walker. I went down hard hitting my left knee, the right palm of my hand bending back my wrist and hitting my chin on the pavement. I jerked my neck and lower back. Of course I twisted my ankle and foot as well. My knee, hand and chin were bleeding as I hobbled back to the house. Over the week the pain in the knee that I skinned began to turn into burning RSD type pain and was mirrored in the opposite knee. This was one of the few places that I hadn't had RSD before. My right wrist, which I had had injected for my carpal tunnel syndrome a month ago was now hurting worse than before the injection and was numb most of the time. I pulled something in my left shoulder, was having muscle spasms in my neck and sciatica in my back shooting down into my right buttocks. The next day I went to my PCP and got a muscle relaxant. Because I was going to have Ketamine in less than I week, I couldn't take my Nucynta. Opiates block the receptors that Ketamine binds to preventing it from doing it's job to reboot the nervous system. They should not be taken any closer than two weeks before the beginning of the Ketamine infusion.
Sunday March 25th, I met Christina for the first time when she arrived at my house to drive to Miami with me. Most doctors require that you have someone with you after your Ketamine infusions. Since my husband travels for work during the week; Christina was kind enough to offer to drive down with me and stay with me in Miami while I had my Ketamine Monday through Friday.
Our adventure began about 3:45 after loading my car with our luggage. Fortunately there wasn't much traffic. We had an enjoyable drive getting to know each other. We stopped for a quick bite to eat just about half way there. We arrived at the Spring Hills Suites, which was just a couple of blocks from the Sylvester Cancer Center of the University of Miami Jackson Medical Center just after dark.
The protocol that Dr Patin was going to use was Dr S's since I had been inpatient with Dr S and these were supposed to be my follow up "boosters". Even though the timing was off, Dr Patin felt that he should follow the dosages that Dr S uses in his post inpatient protocol for his set of 5 infusions. After this week, we could talk about using Dr Patin's protocol.
Monday morning my infusion started over two hours late. I have a port for my infusions. Even though it is a cancer center with a pain management department within it; they had to search for a nurse from the chemotherapy area who was port certified who could access my port. My pain management anesthesiologist, Dr Patin, had his resident doing a one on one with me during my infusion. This was her first infusion. Although she was already a pediatrician, she had decided to go back and do an anesthesiology residency. Once the port was accessed, it took them a while to get me hooked up the the monitor, get the Ketamine and get things started. The recovery room nurses were extremely busy by the time the drugs were in the unit and it was up to the resident to calculate the rate of the IV. It was a 100 cc bag that was to run over a 4 hour period. To calculate the rate per hour of the infusion you divide 100 by 4 and get a rate of 25 cc per hour. Well some how she recalculated the dose, which was already calculated in the 100 cc bag. There were 200 mg of Ketamine in that 100 cc of fluid. Any how she came up with a rate of 0.5 cc per hour. I politely asked her if I could check her calculations and she declined. She put me behind the curtain and had things situated so that only the monitor could be seen. She didn't give me the call bell either. By the time one of the nurses came over to check on her; nearly half of the infusion time had gone by and only 1 cc of the 100 ccs in the bag had been infused. Of course the nurse noticed the mistake and paged Dr Patin who was in the clinic seeing patients. Dr Patin decided that since I had had the coma Ketamine and so much Ketamine over the last 10 years that it would be ok to run the entire 200 mg over the remaining 2 1/2 hours rather than starting over and going for 4 more hours. He set the rate at 75 cc/hr (triple what it was originally supposed to be) and gave me extra Versed. For the first time ever, during that infusion I had a hallucination. Not even during my coma did I have a hallucination. I knew that this was what it was while I was having it so I wasn't frightened. I could see and hear what was happening within the room so the hallucination was a distortion of what was going on in the recovery room with people flying around. When the infusion was over, there are a few things you must do before they release you: drink something, go to the bathroom and sit in the recliner for a set amount of time. As soon as they gave me some water, I got very nauseous. Before the zophran was delivered from the pharmacy, I was vomiting. When Dr Patin came to check on me my speech was very slurred. I had to stay and recover for over an hour when I'm usually ready to leave within half an hour at the most. Christina walked me up to our room and went out to get food as I was not steady enough to go out to dinner that night. We didn't want to take any chances on me falling.
Tuesday, Dr Patin continued following Dr S's post inpatient protocol of 200 mg. We got started late again but my port was still accessed from Monday. The resident knew where the supplies were and so the delay wasn't too long. For the remainder of the week, she made sure that she had Zophran and gave it to me at the beginning of the infusion since it last for 6 hours. The IV pump was set to the correct rate so I was wide awake during the infusion listening to music. After the infusion I was able to speak to Dr Patin at length. I gave him an article that I brought from home on Ketamine nasal spray, spoke with him about his RSD experience and told him about my involvement with the Ketamine Klub. He was interested in learning more about the Ketamine nasal spray and asked if I minded if he did prescribe it for me if it was approved if it would be ok to have it made at his compounding pharmacy and mailed to me. That was fine with me since I don't know of a local compounding pharmacy. I learned that he has been doing Ketamine infusions for a while but with cancer pain patients. He has minimal RSD experience but was willing to listen, read and learn more. I contacted one of our K Klub members and she volunteered to print some specific articles and bring them to me later in the week to give them to Dr Patin.
Wednesday we continued with the 200 mg protocol. Things started closer to 8:00 and went without a hitch. I was still having pain in my knees, wrists, and sciatic nerve in addition to my usual places. I decided that I needed to ask Dr Patin to forget about Dr S's protocol since my pain was as bad as it was before Dr S put me into Hahnemann for my inpatient. We only had two days left to squash this new pain or risk it being a permanent spread.
Thursday while they were getting set up, I had a visit from a fellow RSDer who works at U of Miami Medical. I told the resident that there had been no change in my pain and that she needed to speak to Dr Patin (who was in a procedure) about increasing the dosage since we only had two infusions left. After Talia left, I closed my eyes as I had come down with a cold and was feeling rather lousy. I hadn't slept the night before. All of a sudden I could tell that there had been a change. Unlike Tuesday and Wednesday, I was starting to feel a bit loopy. I asked the resident if anything had changed. She said that she had reached Dr Patin between procedures and that she had doubled the dose from 200 mg to 400 mg over the 4 hour infusion. On the stretcher with me I had a box of tissues, a plastic bag to put the used ones in and my cell phone. Some how my phone dialed my friend Tara (who lives in Syracuse NY) who is my health care proxy. I sounded like a drunk. She asked me if there was someone else that I could give the phone to. On my left, I was up against a wall. On my right the curtain was closed. In front of me the curtain was closed. The resident could only see the monitor and once again she hadn't given me the call bell so I said no. I assured her that everything was fine and that they had just increased my dose. My husband Jim was traveling back home so she couldn't get him on the phone to find out what was going on so she left him a message saying nothing urgent because she knew that if he even saw her number he would panic. As soon as the infusion was over; fortunately I remembered the conversation so I texted her and apologized for the phone call and explained that I had been wide awake which is why I had the phone with me to listen to music. Thursday evening, another one of my RSD Facebook friends and her husband met up with Christina and I for dinner. She was kind enough to have printed out articles for me to give to Dr Patin on Friday for him to read specifically about RSD and about Ketamine results on RSD patients. We had a wonderful dinner talking about RSD, Ketamine and coincidentally Georgiana's mom has Parkinson's and my father died of ALS. Twelve years ago when my father was diagnosed at John's Hopkins the neurologists there told me that there was absolutely no possibility that there was any correlation between my RSD and my father's ALS. It just seemed like too much of a coincidence that we would both have a neuromuscular disease. Now they think that there might be a connection between MS, Parkinson, ALS and RSD.
Friday I again got a late start but was able to get the 400 mgs over 4 hours. This time I left my cell phone in the bag with my clothing so that there would be no accidental calls. I was already out when Talia stopped by to say hello. After the infusion, Dr Patin came to talk again. It was very obvious that he had read the article on Ketamine nasal spray and gladly took the articles that Georgiana printed for me. We spoke for about half an hour before his assistant came to get him because he had someone waiting in his office for him.
Right now he has staffing issues but he has been told by the administration that if he gets a Ketamine patient base that they will give him three dedicated beds and his own nurse in the anesthesia recovery room. Right now, he can only do one patient at a time so it would be a huge improvement to be able to do three at a time and to have a nurse doing the infusions rather than a different resident each month. Although cancer pain is his specialty, he really knows ketamine and is willing to do high dose Ketamine as high as 4 mg/kg/hr over 6 hours with a 2 - 3 hour recovery period. That is the same dose that I got in Germany during my coma. The difference is of course that during my coma the Ketamine ran 24 hours a day for 6 days rather than 6 hours a day for 5 days. He has the experience working with pain management and he seems willing to learn about RSD. Unlike most pain management doctors in FL, he is not opposed to his RSD patients having a local pain management doctor or RSD specialist and using him for their Ketamine only.
I feel that once he builds up his patient base and gets the extra staff that this could be a really good thing for those of us in the southeast. Right now there are kinks and we will have to be patient while they work them out. The nurses couldn't have been nicer or harder working. I never saw them sitting down for a minute except for when they were making their follow up calls from the previous day's cases.
At this time, Dr Patin does not do inpatient Ketamine as he works in the Cancer Center; however I did hear that there is another pain management doctor at the U of Miami hospital which is 5 blocks away who does do inpatient Ketamine. I'm working on getting that information.
There is a nice hotel (Spring Hill Suites) just a couple blocks away from the Sylvester Cancer Center. I suggest that you make your reservations as far in advance as you can. If you can't get in there, you'll have to choose a hotel near the airport which isn't too far away but I suspect would be noisier. There is a free breakfast at Spring Hill Suites but of course the one getting the Ketamine won't be able to eat breakfast. We found a couple of good places to eat including Greek and Cuban. There was also a Winn Dixie within a couple of blocks. The Spring Hill Suites has a microwave and a mini-refrig. There is also a small pool for the person accompanying the RSDer. Parking at the hotel is $15/day plus $3 tax. They charge for parking at the caner center too but what we did was to have me call when they called transport to take me out to the pick up area. Christina would leave the hotel then and most of the time we would both arrive out front at the same time. This way we wouldn't have to pay to park at the cancer center in addition to the hotel.
This week of infusions really saved me since I'd fallen but unfortunately it didn't take care of my "normal" pain. It is Dr Patin's protocol to have the infusions every three months but I'm not sure that I will make it three months which is ironic because after my 2009 inpatient and follow up, I didn't have another infusion until I went inpatient in late January of this year. That admission was prompted by a bad fall October 30th 2011.
Thursday I am meeting with a podiatrist to look at the stability of my foot and ankle to see if there is anything that we can do to decrease my fall risk without the use of a cane/walker keeping in mind that I can't tolerate a shoe. I can wear a sandal but nothing that touches the top of my foot where the surgical scars are. We'll see how that goes.
If anyone has any questions about Dr Patin or the Sylvester Cancer Center, feel free to ask them in the comments or to email me at nrcotterman@yahoo.com.
Saturday, March 31, 2012
RSD and the Health Continuum
RSD and the Health Continuum
When we were in nursing school, we were taught that our health was more like a continuum with illness on one end and wellness on the other end like this:
Now the balance of this continuum depended on our state at the time. Our normal situation could vary. For instance, if someone were diagnosed with a permanent condition such as RSD, then this would be their normal or where they stand as in fair, average or good health. The continuum would shift in the direction of average to good health from fair to poor health as this condition becomes our new normal. If I caught the flu or got cancer on top of my RSD then the balance would shift towards fair, poor, very poor or even extremely poor depending on my prognosis or even though I still had RSD because in addition to the RSD, I was sick. Some people would consider RSD being sick but for me, this is my normal. If I were to have an exacerbation or flare up of my RSD that was out of my normal for my RSD, then this continuum would again tip towards the below average, to fair side.
Health is not black and white. I can still have this “abnormal” condition and still in good health for me for me one day and be sick or in below average or in poor health another either with something different like a cold, the flu or even an exacerbation of my RSD.
If you think of RSD in this way, it is easier to integrate it into your daily life and not think of yourself as a “sick person” every day but realize that this is part of your every day life and help to accept RSD. I’m not saying that we will ever forget that we have it. What I am saying is that it can’t be the center of our lives. Until it isn’t and we find other things to do and other intests in our lives; we truly won’t be healthy.
Now the balance of this continuum depended on our state at the time. Our normal situation could vary. For instance, if someone were diagnosed with a permanent condition such as RSD, then this would be their new normal/well. The continuum would shift in that direction. If I caught a could then the balance would shift towards sick even though I still had RSD because in addition to the RSD, I was sick. Some people would consider RSD being sick but for me, this is my normal. If I were to have an exacerbation or flare up of my RSD that was out of my normal for my RSD, then this continuum would again tip towards the sick side.
Health is not black and white. I can still have this “abnormal” condition and still be well for me one day and be sick another either with something different like a cold, the flu or even an exacerbation of my RSD.
If you think of RSD in this way, it is easier to integrate it into your daily life and not think of yourself as a “sick person” every day but realize that this is part of your every day life and help to accept RSD. I’m not saying that we will ever forget that we have it. What I am saying is that it can’t be the center of our lives. Until it isn’t and we find other things to do and other interests in our lives; we truly won’t be healthy.
Wednesday, February 15, 2012
IV Access in Ketamine Infusion Therapy
I.V. Access For Ketamine Infusion
informed Consent
When you have made the decision to get IV Ketamine; you need to make an educated (informed) decision as to how the Ketamine should be infused into your body. This decision needs to be made in conjunction with your doctor.
For the most part, when you enter into treatment with Ketamine for RSD, it is an ongoing treatment if it is successful. This should be taken into consideration when deciding what type of IV access you want.
If your first Ketamine treatment is outpatient and you are not sure how it will work for you; as Ketamine is not always the best treatment for everyone, then a traditional peripheral IV may be your best access. The peripheral IV must be changed every 72 hours (in most institutions). When you are getting outpatient treatments, most facilities will allow you to go home with it in place for three days of outpatient infusions. They will take steps to protect the catheter when you are at home so that it doesn’t get dislodged. There is always the chance that it will become dislodged and need to be replaced. Lidocaine (a numbing medication) can be used when a peripheral IV is started. There have been some cases where the placement of an IV has caused spread of RSD. I could not find any percentages of cases where the spread of RSD was associated with an IV stick. Here is what a peripheral IV looks like:
If your first Ketamine treatment is inpatient; you will most likely be getting follow up “booster” infusions (infusions in an outpatient setting). In this case, it makes more sense that you get a more permanent access. One form of permanent IV access is a mediport/portacath. This is surgically implanted, usually in your chest just under the skin, and is accessed by a special needle called a Huber needle. When the port is not being used, it is just a slight bulge under the skin. When it is being used, the Huber needle is inserted into a reservoir just under the skin and secured with a clear dressing. The Huber needle can stay in place for up to seven days. The risk of infection is very low with this type of device. It does require monthly flushing by a nurse to keep it patent. This can be done in your doctor’s office. Here is some information on the mediport/portacath:
Some Benefits Of The Mediport/Portacath System Include:
- It minimizes damage to veins, muscle and skin tissue by allowing the medication to be diluted faster in the larger veins
- It allows for a single location that your doctor can use to infuse Ketamine and/or take blood directly from large veins.
- It avoids the risk and pain to the RSD patient of looking for new veins each time the patient needs an infusion or have a blood sample taken.
- Scar tissue builds up over time at the Mediport/Portacath location making each needle penetration less painful over time.
- Minimizes risk of infection over a temporary central line.
- Can be left in place for years with proper maintenance (monthly flushing)
There are other central line options that include a PICC line (peripherally inserted central line) which is inserted in the arm, a Hickman, and a non-tunneled central line which are also inserted in the chest area. Here is a Wikipedia explanation of some other types of central lines. Most of these types of central lines are temporary in nature and are removed before you are discharged from the hospital or are left in for only a short time after discharged unlike the Mediport/portacath which can be left in place for years.
As you can see, if you are going into the hospital for inpatient Ketamine therapy, how the Ketamine is going to be infused is something that you need to think about and discuss with your physician BEFORE you are admitted. You don’t want to find out the morning of admission that you are getting a different type of IV access than you thought or that you are getting removable sutures rather than dissolvable sutures and steri-strips. You don’t want to find out upon discharge when you are sleepy and possibly still disoriented that your IV access is being removed; when you thought that it was staying in place for future infusions.
This is just another part of your informed decision that you need to make when planning your RSD Ketamine treatment.
Friday, February 10, 2012
Inpatient Ketamine Experience 2012
January 29, 2012 I began my journey to Philadelphia for my fifth ICU inpatient Ketamine infusion at Hahnemann Hospital. I flew from Orlando to Philadelphia where my youngest cousin Joyce and her middle daughter Ainsley picked me up at the airport and took me to my center city hotel.
Although Joyce is 18 years my junior (and her daughter 50 years my junior almost to the day); of my first cousins she and I am probably the closest as adults as I am to any of my adult cousins. It was great to have that time to catch up to her. Once I got settled into my hotel, I got a visit from a high school friend (Donna) who I hadn't seen in close to twenty years. It was nice to have a one on one chat to catch up. Shortly thereafter, a RSD friend (Diane) who I've never met in person, arrived at the hotel to take bring me a pizza steak (a Philly special that we don't get in FL made by her son!) and to take me to supposedly meet some other friends at RAW in center city. We had time for the three of us to chat before we had to leave for the restaurant. It was as if we'd always known each other through our interactions on a Facebook group for people with RSD looking for information and support on Ketamine. (Ketamine Klub for CRPS/RSD Patients)
At 5 p.m. Diane and I headed over to RAW, expecting a party of 10. By 6:00 we realized that it was only going to be the two of us, so we had a very nice dinner together. Although Diane and I had a great dinner, I have to admit that I was really disappointed that old friends and family member didn't make it over to RAW. I alway say that the people in Philly are so much more friendly than here in Orlando. In the 5 1/2 years that we've lived here, I really don't feel like we have any friends here; so I was really disappointed that only one friend and one virtual stranger came to see me in addition to my cousin Joyce who picked me up from the airport. I guess I have too high of expectations of people.
After dinner, Diane headed home. It was a long anxious night for me. Although I had had coma Ketamine twice, inpatient Ketamine at Hahnemann four times before (as well as multiple other ICU stays at Hahnemann for other treatments as well as regular admissions on their neurology floor) and dozens of outpatient Ketamine infusions; I was very anxious about my upcoming admission. I think that no matter how familiar you are with the procedure; going into the hospital, especially the ICU is frightening or at least anticipation of it is unnerving. Perhaps even more so if you are a RN and know all of the things that can potentially go wrong.
It was a very long sleepless night. The Thursday before, I had received a call from Hahnemann's admissions office telling me that I would receive a call early in the morning telling me to come into the hospital and to report to the 4th floor. At 5 a.m. I accessed my portacath. This is an IV port in my chest that provides IV access. No, it is not normal for the patient to access their own port. It is something that I am anal about. I have always done my own port care since one was placed in 1999. I know that my sterile technique is excellent. I guess it is something that I have some control over in a situation that a patient has very little control. Before every hospitalization or procedure, I always access my own port. I like a specific needle and I'm allergic to the Tegaderm that most facilities use (I use Op-site which most facilities don't have and my IV equipment provider provides for me). I also have experienced long waits while the hospitals find a nurse who is port certified to access the port upon admission; so I've gotten into the habit of going into the facility with it already accessed using my own equipment.
I waited and waited and no phone call. RSD Facebook friends started texted me..."any call yet?". No call. It was 7:00 a.m. and no call. I knew that the other Ketamine patient had to go to the OR and get a port put in (something I only knew because of our Facebook group otherwise I wouldn't have even known what was going on with the other Ketamine patient due to HIPPA laws. My doctor has 2 ICU beds held every week for an inpatient Ketamine admission). 8:00 came and I decided to call admissions. They said that there was no bed available and they'd call me. I doubted that this was so since normally the Ketamine patients are discharged on Sundays. Most likely it was that the nurses weren't ready for an admission. Finally at 9:30, I decided just to check out of the hotel get a cab and go over to the hospital and wait there as I was going crazy in the hotel room (which was freezing and had no separate thermostat for the rooms). I went down to the desk and checked out. They got me a cab for the three block ride to Hahnemann but my body was now used to FL weather and I just couldn't handle the walk around City Hall dragging my luggage in the cold to Hahnemann. I had to go to admissions on the first floor to sign a paper that said that if my Blue Cross didn't cover my Medicare Co-pay (which it had in each of my other admissions) then I would pay the difference. Just as I was signing the paper, my cell phone rang and it was admissions calling to ask how soon I could be there. I told them now. So they said to report to the 4th floor; room 405. They didn't say that it was direct admissions. This part had all changed since my last admission in 2009 when you checked in on the first floor admissions where I was at the time.
I made a quick call to my husband knowing that it would be the last phone call that I'd be permitted to make until my discharge, texted my two daughters who were at work by then and unable to accept phone calls and texted one of the administrators of our Facebook RSD group to let them know that I was finally being admitted so that they could post it to the group. I then put my phone on airplane mode so that it could act as my iPod for music and not a cell phone any longer and headed towards the elevators that I had taken from the first floor dozens of times before. I'd always made that trip alone as even when I lived in Philly, I'd always been dropped off at Hahnemann either because my husband was out of town and I'd taken a cab into town or my husband dropped me off early and went to work and I just waited in admissions until they had a bed.
When I got to the fourth floor, there was no room 405. I looked perplexed and someone asked if I needed help (they saw me dragging a huge suitcase as I had to have everything I needed for both hotel stays plus the hospitalization with me). I told her that I was looking for room 405 and she had no idea what I was talking about. I spotted a sign that said "direct admissions" and told her that this was most likely where I belonged. If there was a room number then it was most likely on the open door and not visible. I went into the room and the admission process began. For whatever reason, I became more at ease. Talking to the admitting nurses and being in "my element" made me more at ease; as crazy as that sounds.
Once they did all of their paper work and vital signs there was the long wait for the transportation team to take me in a wheel chair up to the ICU. I find this sort of ironic since I walked from the first floor admissions office, where I signed the form that they needed, up to the direct admissions office but policy doesn't permit you to walk from the direct admissions office to the ICU. That's hospital policy for you!! I was taken to a room without windows that was smaller than the clothes closet that my husband and I share in our bedroom. There was a bed, a chair and a tiny sink for the staff. That is it. It was directly behind the nurses' station so it was very noisy. I had to keep asking everyone who came in and out to close the door or I could hear everything that the staff was saying. The only light was a fluorescent light directly over the bed and extremely bright. Of course I couldn't control the light or the volume on the TV because the control was broken.
Blood work, and EKG and chest x-ray (to check port placement on a port that's been in place since 2007 and they'd already taken blood from) were all done. The critical care nurse practitioner (NP) came in and introduced herself, took a history and did an exam. She explained that it would be her team that would follow my care in the ICU. Next the neurology chief resident came in and did his assessment and explained that Dr S would be in later. There were residents, nurses, techs, etc. in and out all afternoon. Finally I asked if I was ever going to get lunch. The nurse said, "oh that came up hours ago, let me order you something". Of course breakfast in the hotel was at 6:00 a.m. - 7:00 a.m. because it was meant for businessmen so I was starving.
Eventually IV fluids were hung and potassium hung because my potassium is always low when I'm hospitalized but normal when they check it as an outpatient because they use different values inpatient than outpatient. This was an issue though out the hospitalization. Once the Ketamine was hung, you can't give IV potassium as it is incompatible with IV Ketamine. Since my potassium continued to be low in spite of multiple dosages, they had to keep giving it to me orally, first as a horrible liquid. I then asked why they couldn't give it to me in pill form; as I knew that it came in a pill form. The nurse asked if I as good at swallowing pills? I said yes, so for the rest of the week, I got the potassium in pill form. I'm sure my level never reached the inpatient level because it never does. I predicted it to the admitting nurse when she drew my initial labs. It is so stupid that there is a difference between the levels inpatient and outpatient and that they are so anal about the slight difference.
Finally in the late afternoon everything was in place to start the Ketamine. The nurse could hang the bag, but the doctor had to actually push the start button on the IV pump. IV Versed was pushed and I was told that there was a shortage of IV Ativan so that I would have to take that by mouth. Let the fun begin!! They start the Ketamine out at 10 mg per hour and increase it by 10 mg per hour every hour until you reach 40 mg per hour where it remains for the next five days.
Now, I have mentioned before that I have had a lot of Ketamine over the last ten years and I have developed quite a tolerance. Most people feel a bit tipsy or goofy when the Ketamine gets to the 40 mg per hour; at least that is how it has been described to me. It doesn't have that affect on me. I am able to have a perfectly rational conversation with someone at that level. The reason that they do not allow patients to have cell phones or computers while on Ketamine at Hahnemann is because they may do something goofy that they may regret later. If you are caught with a cell phone, it will be confiscated (I found that out in 2009 when I tried to call my husband). This time, I explained to the nurses that although this was an iPhone, it was on the airplane mode so that it couldn't be used as a phone and that I was using it as an iPod. It is acceptable to have an iPod to listen to music during your Ketamine infusion.
Immediately after being given the IV Versed, I would get a little bit sleepy, but it didn't last long and with all of the noise and interruptions, I really didn't sleep. One of the precautions that was taken was that an ultrasound tech did an ultrasound of both legs to check for blood clots. Being immobile (and long plane flights) can predispose you to blood clots which can travel to your heart and lungs and be fatal. This ultrasound tech lived in the Orlando area near my home for a while. There was a particular incident that happened in my subdivision in 2007 when we both lived here. During my ultrasound, we were discussing it in great detail. Eventually she made a notation about how I was able to hold a rational detailed conversation in my chart as most of the Ketamine patients sleep during her exam. When Dr S made his rounds that evening, he asked me if I wanted to see a friend of mine who works with him. I said "I've known him for 29 years". His response was "my wife has known me for 42 years but that doesn't mean that she wants to see me". To which I answered "let me rephrase that; we've been good friends for 29 years, of course I want to see him." That confirmed that I was far too awake and rational so he told me that they needed to sedate me with other medications so that I would sleep because I was far too awake. When my friend came in I told him that this might be the last rational conversation that I have for a while because Dr S plans on snowing me. We had a nice visit and it was our only visit but Dr S wasn't really successful in snowing me. With all of the blocks and procedures that I've had over the past years since 1998 when I began treatment for my RSD, I've been given so much sedation that the standard sedation just doesn't snow me.
Additionally, it was arranged for me to have a block to help with the RSD in my face. It was done on the right side of my neck as the RSD on my right side is worse than my left side. It was done right in my ICU bed with the Ketamine running. It wasn't able to be done until Friday due to the doctor's schedule otherwise, he would have injected the other side on another day.
Because I have a neurogenic bladder, I catherize myself 4 times a day. Well the critical care NP assumed that I would be incapable of that, plus they have to have control over things like that; so the nurses had to do it. The nurses would have preferred that I have a foley but the NP was afraid that I would be unable to urinate afterwards and that would hold up my discharge so she wanted me to be straight cathed like normal. Some of the nurses were quite rough. Upon discharge I was quite sore.
I also have very sensitive skin, as do many of us with RSD. I asked that the cardiac leads be rotated. I even gently pulled some of them off so that they had to change them but I still ended up with "burns" on my chest where the leads had been that I am still applying cream to to get to heal.
Back to the Ketamine, Monday through Saturday morning the Ketamine ran at 40 mg per hour, I was given the Versed and Ativan and a routine of catherizations, meals, change of shifts, doctors' rounds, etc. settled in. It seemed as though there was always someone in my room and sleep was very disrupted if at all possible. Again, other people have reported to me that they slept the entire six days and have no memory of the entire hospitalization but this was not my experience this admission nor the admission in 2009. I can tell you every TV show that I watched and every song that I listened to on my iPod.
By Sunday morning, my Ketamine was weaned off (in 10 mg/hr intervals just as it was increased), the IV fluids were discontinued and I was ready to be discharged. It had been arranged that my Mom's sister and her husband would pick me up from the hospital as you need an actual person to be there for discharge and they would drive me to a hotel near the airport. A friend who I've known for 30 years, from Syracuse NY was driving down to stay with me until I would fly home Tuesday. My discharge instructions were no activity for 2 days. When I got to the hotel, my Aunt and Uncle dropped me off around 11:00 a.m. and my friend wasn't due to arrive until 4 p.m. I was starving. I texted my friend Diane who graciously agreed to bring me some food. Since there were no showers and they didn't allow you to wash up with anything other than microwaved antiseptic bath wipes in the ICU, I headed to the shower. That was so exhausting that I laid down for a nap. Having not really slept for a week, I was exhausted.
Ketamine really helps to pull the edema that RSD causes out of your body, plus they are pumping you full of IV fluids. Additionally, I had asked my cousin Joyce to bring me bottled water for the hospital to be sure that I would stay hydrated because hospitals are always dry. Well, in the hotel I didn't have bottled water, slept most of the day/evening/night Sunday and all day Monday forgetting to drink and barely eating. Tuesday I flew home and flying is also dehydrating. Big mistake; because by the time I got home, I wasn't urinating at all; even when catheterizing. I started pushing the water, had my husband get cranberry juice to help my bruised urinary system from the rough catheterizing. Fortunately after 24 hours I was starting to rehydrate myself and avoided being rehospitalized for dehydration.
A word for the wise, if you go for Ketamine, remember as you are sleeping it off after, have someone wake you up on a regular basis and force you to drink a glass of water hourly so that this doesn't happen to you. I never thought to have Amy do it and my husband would never have thought to do it. I figured it out on my own when I was home, but it was almost too late. I had no urine, no tears and probably should have gone into the ER for hydration but any RSDer knows what a nightmare it is for someone with RSD to go into the ER. Since I wasn't vomiting and didn't have diarrhea, I knew that I could hydrate myself orally. Had I experienced one of these two complications, I would have either called my PCP for an order for home IV fluids through my home IV company or gone into the ER for hydration.
The first 48 hours at home, I felt very depressed. Dr S did give me a prescription for Ativan 2 mg to take as needed. I take Ativan for sleep and didn't want to add to my tolerance. Besides Ativan is for anxiety and not for depression and may have added to the depression. I felt that the depression was from coming off of the Versed and Ativan that they were giving me every 4 - 6 hours in the hospital to try to make me sleep. Had I not felt more like my self in 72 hours or if I had any suicidal ideations, I would have called my psychiatrist (who I see every six months to manage my anti-depresion medications) immediately or if it were after hours called a crisis hot line. I know myself very well having dealt with depression since shortly after my accident 16 years ago on March 4th. By Wednesday, I was feeling better. It is very important whether you are receiving inpatient or outpatient Ketamine to monitor your mood because some people do become anxious or depressed. I remember that I felt depressed in the past after Ketamine. I don't think that it is the Ketamine itself as they are now using it to treat depression. I believe that it is the other medications that they give with the Ketamine that when stopped trigger depression.
I hope that by sharing this most recent experience of inpatient Ketamine, it will give those of you who are considering an inpatient Ketamine treatment some idea of what it is like. I am in the process of setting up follow up outpatient infusions here in FL in Miami at Dr S's suggestion rather than traveling back up to Philly on a regular basis.
I have also set up Botox injections for mid-March to see if we can do something for these chronic migraines. Dr S also recommended that I see a hand surgeon about the severe pain caused by my carpal tunnel syndrome to get steroid injections into my wrists. That is scheduled for February 16th.
((((HUGS))) to all
Although Joyce is 18 years my junior (and her daughter 50 years my junior almost to the day); of my first cousins she and I am probably the closest as adults as I am to any of my adult cousins. It was great to have that time to catch up to her. Once I got settled into my hotel, I got a visit from a high school friend (Donna) who I hadn't seen in close to twenty years. It was nice to have a one on one chat to catch up. Shortly thereafter, a RSD friend (Diane) who I've never met in person, arrived at the hotel to take bring me a pizza steak (a Philly special that we don't get in FL made by her son!) and to take me to supposedly meet some other friends at RAW in center city. We had time for the three of us to chat before we had to leave for the restaurant. It was as if we'd always known each other through our interactions on a Facebook group for people with RSD looking for information and support on Ketamine. (Ketamine Klub for CRPS/RSD Patients)
At 5 p.m. Diane and I headed over to RAW, expecting a party of 10. By 6:00 we realized that it was only going to be the two of us, so we had a very nice dinner together. Although Diane and I had a great dinner, I have to admit that I was really disappointed that old friends and family member didn't make it over to RAW. I alway say that the people in Philly are so much more friendly than here in Orlando. In the 5 1/2 years that we've lived here, I really don't feel like we have any friends here; so I was really disappointed that only one friend and one virtual stranger came to see me in addition to my cousin Joyce who picked me up from the airport. I guess I have too high of expectations of people.
After dinner, Diane headed home. It was a long anxious night for me. Although I had had coma Ketamine twice, inpatient Ketamine at Hahnemann four times before (as well as multiple other ICU stays at Hahnemann for other treatments as well as regular admissions on their neurology floor) and dozens of outpatient Ketamine infusions; I was very anxious about my upcoming admission. I think that no matter how familiar you are with the procedure; going into the hospital, especially the ICU is frightening or at least anticipation of it is unnerving. Perhaps even more so if you are a RN and know all of the things that can potentially go wrong.
It was a very long sleepless night. The Thursday before, I had received a call from Hahnemann's admissions office telling me that I would receive a call early in the morning telling me to come into the hospital and to report to the 4th floor. At 5 a.m. I accessed my portacath. This is an IV port in my chest that provides IV access. No, it is not normal for the patient to access their own port. It is something that I am anal about. I have always done my own port care since one was placed in 1999. I know that my sterile technique is excellent. I guess it is something that I have some control over in a situation that a patient has very little control. Before every hospitalization or procedure, I always access my own port. I like a specific needle and I'm allergic to the Tegaderm that most facilities use (I use Op-site which most facilities don't have and my IV equipment provider provides for me). I also have experienced long waits while the hospitals find a nurse who is port certified to access the port upon admission; so I've gotten into the habit of going into the facility with it already accessed using my own equipment.
I waited and waited and no phone call. RSD Facebook friends started texted me..."any call yet?". No call. It was 7:00 a.m. and no call. I knew that the other Ketamine patient had to go to the OR and get a port put in (something I only knew because of our Facebook group otherwise I wouldn't have even known what was going on with the other Ketamine patient due to HIPPA laws. My doctor has 2 ICU beds held every week for an inpatient Ketamine admission). 8:00 came and I decided to call admissions. They said that there was no bed available and they'd call me. I doubted that this was so since normally the Ketamine patients are discharged on Sundays. Most likely it was that the nurses weren't ready for an admission. Finally at 9:30, I decided just to check out of the hotel get a cab and go over to the hospital and wait there as I was going crazy in the hotel room (which was freezing and had no separate thermostat for the rooms). I went down to the desk and checked out. They got me a cab for the three block ride to Hahnemann but my body was now used to FL weather and I just couldn't handle the walk around City Hall dragging my luggage in the cold to Hahnemann. I had to go to admissions on the first floor to sign a paper that said that if my Blue Cross didn't cover my Medicare Co-pay (which it had in each of my other admissions) then I would pay the difference. Just as I was signing the paper, my cell phone rang and it was admissions calling to ask how soon I could be there. I told them now. So they said to report to the 4th floor; room 405. They didn't say that it was direct admissions. This part had all changed since my last admission in 2009 when you checked in on the first floor admissions where I was at the time.
I made a quick call to my husband knowing that it would be the last phone call that I'd be permitted to make until my discharge, texted my two daughters who were at work by then and unable to accept phone calls and texted one of the administrators of our Facebook RSD group to let them know that I was finally being admitted so that they could post it to the group. I then put my phone on airplane mode so that it could act as my iPod for music and not a cell phone any longer and headed towards the elevators that I had taken from the first floor dozens of times before. I'd always made that trip alone as even when I lived in Philly, I'd always been dropped off at Hahnemann either because my husband was out of town and I'd taken a cab into town or my husband dropped me off early and went to work and I just waited in admissions until they had a bed.
When I got to the fourth floor, there was no room 405. I looked perplexed and someone asked if I needed help (they saw me dragging a huge suitcase as I had to have everything I needed for both hotel stays plus the hospitalization with me). I told her that I was looking for room 405 and she had no idea what I was talking about. I spotted a sign that said "direct admissions" and told her that this was most likely where I belonged. If there was a room number then it was most likely on the open door and not visible. I went into the room and the admission process began. For whatever reason, I became more at ease. Talking to the admitting nurses and being in "my element" made me more at ease; as crazy as that sounds.
Once they did all of their paper work and vital signs there was the long wait for the transportation team to take me in a wheel chair up to the ICU. I find this sort of ironic since I walked from the first floor admissions office, where I signed the form that they needed, up to the direct admissions office but policy doesn't permit you to walk from the direct admissions office to the ICU. That's hospital policy for you!! I was taken to a room without windows that was smaller than the clothes closet that my husband and I share in our bedroom. There was a bed, a chair and a tiny sink for the staff. That is it. It was directly behind the nurses' station so it was very noisy. I had to keep asking everyone who came in and out to close the door or I could hear everything that the staff was saying. The only light was a fluorescent light directly over the bed and extremely bright. Of course I couldn't control the light or the volume on the TV because the control was broken.
Blood work, and EKG and chest x-ray (to check port placement on a port that's been in place since 2007 and they'd already taken blood from) were all done. The critical care nurse practitioner (NP) came in and introduced herself, took a history and did an exam. She explained that it would be her team that would follow my care in the ICU. Next the neurology chief resident came in and did his assessment and explained that Dr S would be in later. There were residents, nurses, techs, etc. in and out all afternoon. Finally I asked if I was ever going to get lunch. The nurse said, "oh that came up hours ago, let me order you something". Of course breakfast in the hotel was at 6:00 a.m. - 7:00 a.m. because it was meant for businessmen so I was starving.
Eventually IV fluids were hung and potassium hung because my potassium is always low when I'm hospitalized but normal when they check it as an outpatient because they use different values inpatient than outpatient. This was an issue though out the hospitalization. Once the Ketamine was hung, you can't give IV potassium as it is incompatible with IV Ketamine. Since my potassium continued to be low in spite of multiple dosages, they had to keep giving it to me orally, first as a horrible liquid. I then asked why they couldn't give it to me in pill form; as I knew that it came in a pill form. The nurse asked if I as good at swallowing pills? I said yes, so for the rest of the week, I got the potassium in pill form. I'm sure my level never reached the inpatient level because it never does. I predicted it to the admitting nurse when she drew my initial labs. It is so stupid that there is a difference between the levels inpatient and outpatient and that they are so anal about the slight difference.
Finally in the late afternoon everything was in place to start the Ketamine. The nurse could hang the bag, but the doctor had to actually push the start button on the IV pump. IV Versed was pushed and I was told that there was a shortage of IV Ativan so that I would have to take that by mouth. Let the fun begin!! They start the Ketamine out at 10 mg per hour and increase it by 10 mg per hour every hour until you reach 40 mg per hour where it remains for the next five days.
Now, I have mentioned before that I have had a lot of Ketamine over the last ten years and I have developed quite a tolerance. Most people feel a bit tipsy or goofy when the Ketamine gets to the 40 mg per hour; at least that is how it has been described to me. It doesn't have that affect on me. I am able to have a perfectly rational conversation with someone at that level. The reason that they do not allow patients to have cell phones or computers while on Ketamine at Hahnemann is because they may do something goofy that they may regret later. If you are caught with a cell phone, it will be confiscated (I found that out in 2009 when I tried to call my husband). This time, I explained to the nurses that although this was an iPhone, it was on the airplane mode so that it couldn't be used as a phone and that I was using it as an iPod. It is acceptable to have an iPod to listen to music during your Ketamine infusion.
Immediately after being given the IV Versed, I would get a little bit sleepy, but it didn't last long and with all of the noise and interruptions, I really didn't sleep. One of the precautions that was taken was that an ultrasound tech did an ultrasound of both legs to check for blood clots. Being immobile (and long plane flights) can predispose you to blood clots which can travel to your heart and lungs and be fatal. This ultrasound tech lived in the Orlando area near my home for a while. There was a particular incident that happened in my subdivision in 2007 when we both lived here. During my ultrasound, we were discussing it in great detail. Eventually she made a notation about how I was able to hold a rational detailed conversation in my chart as most of the Ketamine patients sleep during her exam. When Dr S made his rounds that evening, he asked me if I wanted to see a friend of mine who works with him. I said "I've known him for 29 years". His response was "my wife has known me for 42 years but that doesn't mean that she wants to see me". To which I answered "let me rephrase that; we've been good friends for 29 years, of course I want to see him." That confirmed that I was far too awake and rational so he told me that they needed to sedate me with other medications so that I would sleep because I was far too awake. When my friend came in I told him that this might be the last rational conversation that I have for a while because Dr S plans on snowing me. We had a nice visit and it was our only visit but Dr S wasn't really successful in snowing me. With all of the blocks and procedures that I've had over the past years since 1998 when I began treatment for my RSD, I've been given so much sedation that the standard sedation just doesn't snow me.
Additionally, it was arranged for me to have a block to help with the RSD in my face. It was done on the right side of my neck as the RSD on my right side is worse than my left side. It was done right in my ICU bed with the Ketamine running. It wasn't able to be done until Friday due to the doctor's schedule otherwise, he would have injected the other side on another day.
Because I have a neurogenic bladder, I catherize myself 4 times a day. Well the critical care NP assumed that I would be incapable of that, plus they have to have control over things like that; so the nurses had to do it. The nurses would have preferred that I have a foley but the NP was afraid that I would be unable to urinate afterwards and that would hold up my discharge so she wanted me to be straight cathed like normal. Some of the nurses were quite rough. Upon discharge I was quite sore.
I also have very sensitive skin, as do many of us with RSD. I asked that the cardiac leads be rotated. I even gently pulled some of them off so that they had to change them but I still ended up with "burns" on my chest where the leads had been that I am still applying cream to to get to heal.
Back to the Ketamine, Monday through Saturday morning the Ketamine ran at 40 mg per hour, I was given the Versed and Ativan and a routine of catherizations, meals, change of shifts, doctors' rounds, etc. settled in. It seemed as though there was always someone in my room and sleep was very disrupted if at all possible. Again, other people have reported to me that they slept the entire six days and have no memory of the entire hospitalization but this was not my experience this admission nor the admission in 2009. I can tell you every TV show that I watched and every song that I listened to on my iPod.
By Sunday morning, my Ketamine was weaned off (in 10 mg/hr intervals just as it was increased), the IV fluids were discontinued and I was ready to be discharged. It had been arranged that my Mom's sister and her husband would pick me up from the hospital as you need an actual person to be there for discharge and they would drive me to a hotel near the airport. A friend who I've known for 30 years, from Syracuse NY was driving down to stay with me until I would fly home Tuesday. My discharge instructions were no activity for 2 days. When I got to the hotel, my Aunt and Uncle dropped me off around 11:00 a.m. and my friend wasn't due to arrive until 4 p.m. I was starving. I texted my friend Diane who graciously agreed to bring me some food. Since there were no showers and they didn't allow you to wash up with anything other than microwaved antiseptic bath wipes in the ICU, I headed to the shower. That was so exhausting that I laid down for a nap. Having not really slept for a week, I was exhausted.
Ketamine really helps to pull the edema that RSD causes out of your body, plus they are pumping you full of IV fluids. Additionally, I had asked my cousin Joyce to bring me bottled water for the hospital to be sure that I would stay hydrated because hospitals are always dry. Well, in the hotel I didn't have bottled water, slept most of the day/evening/night Sunday and all day Monday forgetting to drink and barely eating. Tuesday I flew home and flying is also dehydrating. Big mistake; because by the time I got home, I wasn't urinating at all; even when catheterizing. I started pushing the water, had my husband get cranberry juice to help my bruised urinary system from the rough catheterizing. Fortunately after 24 hours I was starting to rehydrate myself and avoided being rehospitalized for dehydration.
A word for the wise, if you go for Ketamine, remember as you are sleeping it off after, have someone wake you up on a regular basis and force you to drink a glass of water hourly so that this doesn't happen to you. I never thought to have Amy do it and my husband would never have thought to do it. I figured it out on my own when I was home, but it was almost too late. I had no urine, no tears and probably should have gone into the ER for hydration but any RSDer knows what a nightmare it is for someone with RSD to go into the ER. Since I wasn't vomiting and didn't have diarrhea, I knew that I could hydrate myself orally. Had I experienced one of these two complications, I would have either called my PCP for an order for home IV fluids through my home IV company or gone into the ER for hydration.
The first 48 hours at home, I felt very depressed. Dr S did give me a prescription for Ativan 2 mg to take as needed. I take Ativan for sleep and didn't want to add to my tolerance. Besides Ativan is for anxiety and not for depression and may have added to the depression. I felt that the depression was from coming off of the Versed and Ativan that they were giving me every 4 - 6 hours in the hospital to try to make me sleep. Had I not felt more like my self in 72 hours or if I had any suicidal ideations, I would have called my psychiatrist (who I see every six months to manage my anti-depresion medications) immediately or if it were after hours called a crisis hot line. I know myself very well having dealt with depression since shortly after my accident 16 years ago on March 4th. By Wednesday, I was feeling better. It is very important whether you are receiving inpatient or outpatient Ketamine to monitor your mood because some people do become anxious or depressed. I remember that I felt depressed in the past after Ketamine. I don't think that it is the Ketamine itself as they are now using it to treat depression. I believe that it is the other medications that they give with the Ketamine that when stopped trigger depression.
I hope that by sharing this most recent experience of inpatient Ketamine, it will give those of you who are considering an inpatient Ketamine treatment some idea of what it is like. I am in the process of setting up follow up outpatient infusions here in FL in Miami at Dr S's suggestion rather than traveling back up to Philly on a regular basis.
I have also set up Botox injections for mid-March to see if we can do something for these chronic migraines. Dr S also recommended that I see a hand surgeon about the severe pain caused by my carpal tunnel syndrome to get steroid injections into my wrists. That is scheduled for February 16th.
((((HUGS))) to all
Monday, January 30, 2012
A case a nerves
I'm sitting in a hotel room less than a mile from Hahnemann, too nervous to go get the free breakfast waiting for THE phone call!
Even tough I've done this several times before, I just want to get it started & not be sitting here freezing in this hotel room with nothing to do! I am tempted to just jump in a cab & show up, but as a nurse Iknow how disruptive that Canberra to a Monday morning. First impressions can make or break a hospital stay. So I will sit here impatiently freezing.
I listen to how badly so many other are doing in our group & wonder if I belong here? I know that over time, we get used to the levels of pain that we once thought were unbearable but some how you feel guilty because you've adapted and although the pain is worse than your "norm"; you don 't interprete it in the same way & with the same intensity as those who have had RSD less than...say 10 years.
Is it because we have accepted this level of pain as normal & don't expect it to be any different and only seek treatment when it breaks out of our "norm" or is there another reason? I hope in collecting the stories & perspectives of some of my fellow RSDers over the coming weeks & months to figure some of this out!
Well still no call so I'll get something hot to drink to warm me up then give Hahnemann a call. Did I say how much I hate waiting???
Even tough I've done this several times before, I just want to get it started & not be sitting here freezing in this hotel room with nothing to do! I am tempted to just jump in a cab & show up, but as a nurse Iknow how disruptive that Canberra to a Monday morning. First impressions can make or break a hospital stay. So I will sit here impatiently freezing.
I listen to how badly so many other are doing in our group & wonder if I belong here? I know that over time, we get used to the levels of pain that we once thought were unbearable but some how you feel guilty because you've adapted and although the pain is worse than your "norm"; you don 't interprete it in the same way & with the same intensity as those who have had RSD less than...say 10 years.
Is it because we have accepted this level of pain as normal & don't expect it to be any different and only seek treatment when it breaks out of our "norm" or is there another reason? I hope in collecting the stories & perspectives of some of my fellow RSDers over the coming weeks & months to figure some of this out!
Well still no call so I'll get something hot to drink to warm me up then give Hahnemann a call. Did I say how much I hate waiting???
Sunday, January 22, 2012
The Countdown Begins
One week from today my journey for my next Ketamine treatment begins. I have mixed feelings. No one wants to go into the hospital, no matter what the reason, except perhaps to give birth. As a RN, I know all of the possible complications of an ICU stay and try not to dwell on them.
The fact that this particular treatment requires you to be completely cut off from your family and friends makes it a bit more scary. They do not permit telephones of any kind in the room. Family members can only call the nurses' station to check on you. Visitation is frowned upon as they really want you to just sleep. Computers are not permitted either; so basically you are cut off from the outside world. The reason for this is twofold. The first is that Ketamine is an anesthesia and makes you a bit loopy. Additionally they give you other medications that have sedative side effects to prevent hallucinations that can be caused by the Ketamine. They do not want you to do or say something that you would regret while getting the medication. Secondly, they want you to rest and sleep as much of the time as possible to let the Ketamine do it's job. Outside interference may prevent the Ketamine from giving you the best possible outcome.
Having been this route several times, I understand this. That doesn't make it any easier to not speak to your husband or daughters for six days. As a nurse, I know that due to the decrease in reimbursements by health insurance companies (which by the way don't actually pay for nursing per say) staffing isn't as good as it used to be and nurses are doing more than they used to do; often the nurses are stretched very thin through no fault of their own. When in another situation, I recommend that family members stay with the patient but in this situation it isn't permitted. Loss of control of your environment is a scary situation for everyone.
The part that I am looking forward to is that the evening before my admission, I am getting together with some friends and family at a chinese restaurant in Center City Philadelphia. Some of them are RSD Facebook Friends, some are friends that I grew up with, some are friends I knew when I lived in the area and some are family members. Other than 8 years when I lived in the Syracuse NY area and the 5 1/2 years that I've lived here in FL; I lived my whole life in the Greater Philadelphia Area. There are a lot of things that I miss about the area including many many people, pizza steaks, TastyKakes, Philly Soft Pretzels, hoagies, and much more including the sports teams. The only thing that don't miss is the weather but that's another story.....
The plan is that I'll arrive next Sunday and be admitted Monday. I will be in the ICU at Hahnemann Monday - Sunday if everything goes according to plan being discharged on Sunday. I have a friend coming to stay with me at a local hotel for a couple of days while I regain my strength so that I can fly home Tuesday 2/7/12 to continue my recovery. Ketamine can be very draining as can lying in bed for 6 days doing nothing. It is amazing how lying in bed for 6 days can cause you to become weak.
Hopefully in addition to the increased RSD pain that I've been experiencing since October, my Phila neurologist will be able to pinpoint the reason for my daily headaches (mostly migraines), and come up with a plan to treat my severe carpal tunnel syndrome as people with RSD are not good candidates for the carpal tunnel release. We have a 50% chance of developing RSD in the hand where the release is done. Without the surgery, I will eventually completely lose the use of the right hand (which is the worse one) and then the left (which is not far behind). My FL neurologist is wondering if the release is done with Ketamine followed by the 6 days of inpatient Ketamine would decrease that risk to a reasonable risk. My FL neurologist is not an expert on Ketamine so he is deferring to my Phila neurologist on this subject. Otherwise, my FL neurologist recommends doing nothing.
This week I need to prepare documents that I will need for my admission, such as my Living Will, medication list, an appreciated medical history, a copy of the lab work that I had done last week and then get together the things that I want to take with me. I want to spend as much time as I can snuggling to my dog Nemo as I will miss her. If only hospitals realized that people would recover much better with their pets rather than without! Nemo has to board next week (which fortunately she loves).
Off the subject; today is my youngest daughter's, Kim's, 28th birthday. I don't know where the time went. It seems like only yesterday that I was at Booth Maternity Center having her and yet 16 of her 28 years; I've had RSD. That's more than half of her life she has had a mom that is only partially functional, but still managed to read all of her homework assignments (before the technology that she has now that reads to her) and type for her (before the technology that speaks what she types); so I think that we managed very well. No, I couldn't take her to the barn for her riding lessons. Her grandmother and father did that but they managed to get me to her competitions. I didn't make every parents' night at school (stairs at school were not doable for me) but I made sure that her dad was in town those nights and went to the girls' back to school nights. We managed. One of the funniest things was trying to guide Kim when I was non-weight bearing on crutches (before she had a guide dog). She would accidentally kick the crutch out from under me while we were walking then grab onto me to prevent me from falling. We didn't go out too much during those weeks without help. Fortunately it was only a 6 week period in 1996 unplanned and a planned period in 1997 when I had fusion surgery. The first time around, my car was totaled and I wasn't driving for most of it anyhow. You would have thought that we would have thought it through the second time around.....but we didn't.
I was chatting with my fellow administrators the other day about the grieving process involved in RSD and in any serious or chronic illness and how important it is to go through that process in order to be successful in your treatment. If I get a chance this week. That will be the topic of my next entry because I feel so very strongly that one of the most important things we need to do is to work out our psychological recovery in order for us to have a physical recovery...more on that next time.
The fact that this particular treatment requires you to be completely cut off from your family and friends makes it a bit more scary. They do not permit telephones of any kind in the room. Family members can only call the nurses' station to check on you. Visitation is frowned upon as they really want you to just sleep. Computers are not permitted either; so basically you are cut off from the outside world. The reason for this is twofold. The first is that Ketamine is an anesthesia and makes you a bit loopy. Additionally they give you other medications that have sedative side effects to prevent hallucinations that can be caused by the Ketamine. They do not want you to do or say something that you would regret while getting the medication. Secondly, they want you to rest and sleep as much of the time as possible to let the Ketamine do it's job. Outside interference may prevent the Ketamine from giving you the best possible outcome.
Having been this route several times, I understand this. That doesn't make it any easier to not speak to your husband or daughters for six days. As a nurse, I know that due to the decrease in reimbursements by health insurance companies (which by the way don't actually pay for nursing per say) staffing isn't as good as it used to be and nurses are doing more than they used to do; often the nurses are stretched very thin through no fault of their own. When in another situation, I recommend that family members stay with the patient but in this situation it isn't permitted. Loss of control of your environment is a scary situation for everyone.
The part that I am looking forward to is that the evening before my admission, I am getting together with some friends and family at a chinese restaurant in Center City Philadelphia. Some of them are RSD Facebook Friends, some are friends that I grew up with, some are friends I knew when I lived in the area and some are family members. Other than 8 years when I lived in the Syracuse NY area and the 5 1/2 years that I've lived here in FL; I lived my whole life in the Greater Philadelphia Area. There are a lot of things that I miss about the area including many many people, pizza steaks, TastyKakes, Philly Soft Pretzels, hoagies, and much more including the sports teams. The only thing that don't miss is the weather but that's another story.....
The plan is that I'll arrive next Sunday and be admitted Monday. I will be in the ICU at Hahnemann Monday - Sunday if everything goes according to plan being discharged on Sunday. I have a friend coming to stay with me at a local hotel for a couple of days while I regain my strength so that I can fly home Tuesday 2/7/12 to continue my recovery. Ketamine can be very draining as can lying in bed for 6 days doing nothing. It is amazing how lying in bed for 6 days can cause you to become weak.
Hopefully in addition to the increased RSD pain that I've been experiencing since October, my Phila neurologist will be able to pinpoint the reason for my daily headaches (mostly migraines), and come up with a plan to treat my severe carpal tunnel syndrome as people with RSD are not good candidates for the carpal tunnel release. We have a 50% chance of developing RSD in the hand where the release is done. Without the surgery, I will eventually completely lose the use of the right hand (which is the worse one) and then the left (which is not far behind). My FL neurologist is wondering if the release is done with Ketamine followed by the 6 days of inpatient Ketamine would decrease that risk to a reasonable risk. My FL neurologist is not an expert on Ketamine so he is deferring to my Phila neurologist on this subject. Otherwise, my FL neurologist recommends doing nothing.
This week I need to prepare documents that I will need for my admission, such as my Living Will, medication list, an appreciated medical history, a copy of the lab work that I had done last week and then get together the things that I want to take with me. I want to spend as much time as I can snuggling to my dog Nemo as I will miss her. If only hospitals realized that people would recover much better with their pets rather than without! Nemo has to board next week (which fortunately she loves).
Off the subject; today is my youngest daughter's, Kim's, 28th birthday. I don't know where the time went. It seems like only yesterday that I was at Booth Maternity Center having her and yet 16 of her 28 years; I've had RSD. That's more than half of her life she has had a mom that is only partially functional, but still managed to read all of her homework assignments (before the technology that she has now that reads to her) and type for her (before the technology that speaks what she types); so I think that we managed very well. No, I couldn't take her to the barn for her riding lessons. Her grandmother and father did that but they managed to get me to her competitions. I didn't make every parents' night at school (stairs at school were not doable for me) but I made sure that her dad was in town those nights and went to the girls' back to school nights. We managed. One of the funniest things was trying to guide Kim when I was non-weight bearing on crutches (before she had a guide dog). She would accidentally kick the crutch out from under me while we were walking then grab onto me to prevent me from falling. We didn't go out too much during those weeks without help. Fortunately it was only a 6 week period in 1996 unplanned and a planned period in 1997 when I had fusion surgery. The first time around, my car was totaled and I wasn't driving for most of it anyhow. You would have thought that we would have thought it through the second time around.....but we didn't.
I was chatting with my fellow administrators the other day about the grieving process involved in RSD and in any serious or chronic illness and how important it is to go through that process in order to be successful in your treatment. If I get a chance this week. That will be the topic of my next entry because I feel so very strongly that one of the most important things we need to do is to work out our psychological recovery in order for us to have a physical recovery...more on that next time.
Monday, January 16, 2012
A Fallen RSD Angel
I would like to preface this post by saying that I have the permission of the mother (Leslie) of this fallen RSD Angel (Andrea) to talk about her daughter as at this point, it is still too painful for her to sit down and write her story.
This weekend, I was reading posts in the Ketamine Klub on Facebook (which I am a co-administrator); which is part of my morning routine. I came across a one line post in the middle of a thread. It read "My daughter died from the Ketamine coma treatment". Other than one of my newest administrators, who had only been appointed the day before, no one seemed to have noticed this post. I immediately responded to the post on the thread and sent this mom a person message with my condolences and to let her know that if it wasn't too painful, I would love to hear her daughter's story.
As you know by know, I consider myself one of the "pioneers" in receiving Ketamine (someone else called me that because it sounded better than guinea pig). Well Andrea was also one of the pioneers of Ketamine. She went to Germany in 2002 for a Ketamine coma and was pain free for 19 weeks. Unfortunately, her insurance would not cover the outpatient infusions so she wasn't able to receive follow up Ketamine. Her pain returned and she got sicker.
At some point after her RSD returned, she needed a heart valve replaced which requires that you be on Coumadin for life. Her RSD continued to ravage her body and in 2008 arrangements were made for her to return to Germany for a second coma treatment. It was at that time that the program in Germany was closed and Andrea's dream to return to Germany slipped away.
Andrea always fought for others with RSD. She started an organization called fighting4us. She was always trying to help others. She got RSD from a chipped bone in her foot at age 13 and lived with it for 13 years. Andrea was a fighter herself. Although I never met her, through messaging with her mother, Leslie, I feel as though I knew her. I know that I would have liked her because I admire her already.
In 2009, arrangements were made for Andrea to go to Mexico in February for a second Ketamine coma. The medical staff there knew that she had the valve replacement. Andrea's cardiologist and her Philadelphia neurologist both gave the clearance for the coma treatment. The staff in Mexico knew that Andrea was on Coumadin and that they would need to put her into the Ketamine induced coma and bring her out of the Ketamine induced coma more slowly. While Andrea was in the hospital, she was switched to Heparin (which is normal protocol).
Leslie describes Andrea's coma as being more restless in Mexico than in Germany. She said that she slept peacefully in Germany but appeared frightened in Mexico and had to be restrained because she was thrashing about. As they were about to bring her out of the coma, Leslie states that the family was sent home to rest being assured that Andrea would be brought out of the coma slowly and that the full staff would attend to her. When they arrived in the morning, Andrea was wide awake.
A day and a half after she woke up, Andrea's heart gave out. Andrea passed at 26 years of age on February 11, 2009; far too young. Andrea's cause of death was heart failure. No parent should have to burry their child. No parent should have to watch their child suffer with something as hideous as RSD. Unfortunately, as we all know too well, many children do suffer with RSD. My heart goes out to Andrea's parents for having to do both; watch their beloved Andrea suffer with RSD and having to burry her!
For those of us who have RSD, we know the pain that Andrea suffered in her short life. For those of us who are caregivers: mothers, fathers, spouses of RSDers, we can identify with Leslie and Gus in their intense pursuit to find any relief for their beloved daughter and can't even imagine the pain that her loss must feel like.
I like to think that we go into these extreme treatments, like coma Ketamine, with informed consent, knowing the risks; but do we all really know the ultimate risk of the treatment. Everyone who goes into a treatment is someone's son or daughter, could be someone's mother or father, sister or brother. I am not saying that you should not have these treatments. What I am saying is that you need to be sure that you know what all of the risks are and that you are willing to take the ultimate risk and put your family through the ultimate outcome before you decide to go through this treatment.
Since I am a nurse, I knew what the risks were going into a Ketamine induced coma. I weighed those risks against what the quality of life that I had at the time. When I had the Ketamine coma; there were no other Ketamine options like there are now. There was no inpatient awake. There was no outpatient infusions. I also had faith in the German health care system. My father and uncle were born in Germany and I had distant relatives that still lived there.
Andrea's story has touched my heart for a whole host of reasons. Andrea is one year younger than my oldest daughter. I can't imagine not having been able to spend the past three years with Laura in my life. Andrea spent half of her life fighting RSD and yet helping others fight RSD. From that standpoint, I want to be just like Andrea. Although I never met her, I have thought about her and her family a lot over the weekend.
After my coma in Germany, I spoke to many patients and their families who were considering going to Germany about my experience. I gave them suggestions about what to bring with them, what to expect during the coma treatment in German, etc. It is very possible that I spoke to Andrea or Leslie prior to their trip to Germany. I hope that if I did, I made a positive impact.
Andrea, I hope that your story will cause people to stop and think about all of the risks before they make the decision to go to a foreign country with a less sophisticated health care system than that of the US. Again, I'm not saying that we shouldn't go. I'm saying that we all need to do our homework and know everything that we can about the treatment, the facility, the doctor, the risks, etc. before going to have the treatment. You need to weigh the quality of life that you currently have against the potential risks of the treatments. Ultimately it is your decision and it should be an informed decision.
Perhaps when Leslie and Gus are feeling stronger, they can join us in our fight to get all insurance companies (see the link on the Ketamine Klub to Erin Brockavitz's web page to tell your story) to cover Ketamine here in the US. Had Andrea's insurance company covered her outpatient follow up Ketamine after her trip to Germany PERHAPS (of course there is no way to be sure) it could have held her coma treatment. If, like Jon Haag, coma treatment were available here in the US PERHAPS (again there is no way to know because people die here in the US too) coma Ketamine would be safer. At least, we wouldn't have the expense of paying out of pocket, travel and treatment would be available to more people. The more a procedure is done, the safer it becomes.
Leslie and Gus, thank you for letting me share this little part of Andrea's story. She must have been a remarkable woman. When you have her foundation set up, I would love to share information about that with my readers as well. No parent should have to burry their child and no child should have to endure the horrors of RSD.
This weekend, I was reading posts in the Ketamine Klub on Facebook (which I am a co-administrator); which is part of my morning routine. I came across a one line post in the middle of a thread. It read "My daughter died from the Ketamine coma treatment". Other than one of my newest administrators, who had only been appointed the day before, no one seemed to have noticed this post. I immediately responded to the post on the thread and sent this mom a person message with my condolences and to let her know that if it wasn't too painful, I would love to hear her daughter's story.
As you know by know, I consider myself one of the "pioneers" in receiving Ketamine (someone else called me that because it sounded better than guinea pig). Well Andrea was also one of the pioneers of Ketamine. She went to Germany in 2002 for a Ketamine coma and was pain free for 19 weeks. Unfortunately, her insurance would not cover the outpatient infusions so she wasn't able to receive follow up Ketamine. Her pain returned and she got sicker.
At some point after her RSD returned, she needed a heart valve replaced which requires that you be on Coumadin for life. Her RSD continued to ravage her body and in 2008 arrangements were made for her to return to Germany for a second coma treatment. It was at that time that the program in Germany was closed and Andrea's dream to return to Germany slipped away.
Andrea always fought for others with RSD. She started an organization called fighting4us. She was always trying to help others. She got RSD from a chipped bone in her foot at age 13 and lived with it for 13 years. Andrea was a fighter herself. Although I never met her, through messaging with her mother, Leslie, I feel as though I knew her. I know that I would have liked her because I admire her already.
In 2009, arrangements were made for Andrea to go to Mexico in February for a second Ketamine coma. The medical staff there knew that she had the valve replacement. Andrea's cardiologist and her Philadelphia neurologist both gave the clearance for the coma treatment. The staff in Mexico knew that Andrea was on Coumadin and that they would need to put her into the Ketamine induced coma and bring her out of the Ketamine induced coma more slowly. While Andrea was in the hospital, she was switched to Heparin (which is normal protocol).
Leslie describes Andrea's coma as being more restless in Mexico than in Germany. She said that she slept peacefully in Germany but appeared frightened in Mexico and had to be restrained because she was thrashing about. As they were about to bring her out of the coma, Leslie states that the family was sent home to rest being assured that Andrea would be brought out of the coma slowly and that the full staff would attend to her. When they arrived in the morning, Andrea was wide awake.
A day and a half after she woke up, Andrea's heart gave out. Andrea passed at 26 years of age on February 11, 2009; far too young. Andrea's cause of death was heart failure. No parent should have to burry their child. No parent should have to watch their child suffer with something as hideous as RSD. Unfortunately, as we all know too well, many children do suffer with RSD. My heart goes out to Andrea's parents for having to do both; watch their beloved Andrea suffer with RSD and having to burry her!
For those of us who have RSD, we know the pain that Andrea suffered in her short life. For those of us who are caregivers: mothers, fathers, spouses of RSDers, we can identify with Leslie and Gus in their intense pursuit to find any relief for their beloved daughter and can't even imagine the pain that her loss must feel like.
I like to think that we go into these extreme treatments, like coma Ketamine, with informed consent, knowing the risks; but do we all really know the ultimate risk of the treatment. Everyone who goes into a treatment is someone's son or daughter, could be someone's mother or father, sister or brother. I am not saying that you should not have these treatments. What I am saying is that you need to be sure that you know what all of the risks are and that you are willing to take the ultimate risk and put your family through the ultimate outcome before you decide to go through this treatment.
Since I am a nurse, I knew what the risks were going into a Ketamine induced coma. I weighed those risks against what the quality of life that I had at the time. When I had the Ketamine coma; there were no other Ketamine options like there are now. There was no inpatient awake. There was no outpatient infusions. I also had faith in the German health care system. My father and uncle were born in Germany and I had distant relatives that still lived there.
Andrea's story has touched my heart for a whole host of reasons. Andrea is one year younger than my oldest daughter. I can't imagine not having been able to spend the past three years with Laura in my life. Andrea spent half of her life fighting RSD and yet helping others fight RSD. From that standpoint, I want to be just like Andrea. Although I never met her, I have thought about her and her family a lot over the weekend.
After my coma in Germany, I spoke to many patients and their families who were considering going to Germany about my experience. I gave them suggestions about what to bring with them, what to expect during the coma treatment in German, etc. It is very possible that I spoke to Andrea or Leslie prior to their trip to Germany. I hope that if I did, I made a positive impact.
Andrea, I hope that your story will cause people to stop and think about all of the risks before they make the decision to go to a foreign country with a less sophisticated health care system than that of the US. Again, I'm not saying that we shouldn't go. I'm saying that we all need to do our homework and know everything that we can about the treatment, the facility, the doctor, the risks, etc. before going to have the treatment. You need to weigh the quality of life that you currently have against the potential risks of the treatments. Ultimately it is your decision and it should be an informed decision.
Perhaps when Leslie and Gus are feeling stronger, they can join us in our fight to get all insurance companies (see the link on the Ketamine Klub to Erin Brockavitz's web page to tell your story) to cover Ketamine here in the US. Had Andrea's insurance company covered her outpatient follow up Ketamine after her trip to Germany PERHAPS (of course there is no way to be sure) it could have held her coma treatment. If, like Jon Haag, coma treatment were available here in the US PERHAPS (again there is no way to know because people die here in the US too) coma Ketamine would be safer. At least, we wouldn't have the expense of paying out of pocket, travel and treatment would be available to more people. The more a procedure is done, the safer it becomes.
Leslie and Gus, thank you for letting me share this little part of Andrea's story. She must have been a remarkable woman. When you have her foundation set up, I would love to share information about that with my readers as well. No parent should have to burry their child and no child should have to endure the horrors of RSD.
A Fallen RSD Angel
Let me preface this post by saying that I have permission from the mother of this fallen RSD Angel to talk about her; as at this time it is still too painful for her to put pen to paper so to speak.
This weekend on our Ketamine Klub page, I saw a posting that made my heart sink. There was a one line post. "My daughter died from this
This weekend on our Ketamine Klub page, I saw a posting that made my heart sink. There was a one line post. "My daughter died from this
Friday, January 6, 2012
Tuesday, January 3, 2012
A more recent Ketamine Article and preparations for Ketamine
As most of you know, I'm going in to Hahnemann later this month for Ketamine. I've had Ketamine over the past 10 years and have been in on it from the start at Hahnemann. I found this article that I found very informative.
http://crps.physiciansforpatients.com/do/articles/81
Today I made my reservations for my flights and hotels. I arranged for a "care taker" for the few days that I am in Philly after I'm discharged. Now I will be putting together my music and hospital kit. I've been working on getting over bronchitis and a sinus infection which hopefully I've finally beat. Now the weather has gone from warm and sunny to cold and windy so I will most likely stay inside until this wintery weather passes. The good thing about Florida is that winter weather doesn't last long. We get big swings in temperature in the winter but it doesn't last long. The swings reak havoc on migraines and RSD but I guess that it is better than sustained cold weather. I need to concentrate on staying well, getting blood work and an EKG done and preparing some meals for my return next month. I'm sure that my hubby will be traveling while I'm in Philly so I will have to board my little Nemo. Fortunately she loves the place that she boards and I know that they will spoil her. If my mom weren't wintering in the FL Keys I would bring her up and she would stay there. That's what we did in 2009 when I was inpatient at Hahnemann.
Now that the holidays are over, my focus will be on getting prepared for my trip to Philly and on getting myself back in better health!
http://crps.physiciansforpatients.com/do/articles/81
Today I made my reservations for my flights and hotels. I arranged for a "care taker" for the few days that I am in Philly after I'm discharged. Now I will be putting together my music and hospital kit. I've been working on getting over bronchitis and a sinus infection which hopefully I've finally beat. Now the weather has gone from warm and sunny to cold and windy so I will most likely stay inside until this wintery weather passes. The good thing about Florida is that winter weather doesn't last long. We get big swings in temperature in the winter but it doesn't last long. The swings reak havoc on migraines and RSD but I guess that it is better than sustained cold weather. I need to concentrate on staying well, getting blood work and an EKG done and preparing some meals for my return next month. I'm sure that my hubby will be traveling while I'm in Philly so I will have to board my little Nemo. Fortunately she loves the place that she boards and I know that they will spoil her. If my mom weren't wintering in the FL Keys I would bring her up and she would stay there. That's what we did in 2009 when I was inpatient at Hahnemann.
Now that the holidays are over, my focus will be on getting prepared for my trip to Philly and on getting myself back in better health!
Subscribe to:
Posts (Atom)